
Osteoporosis Isn’t Exclusive to Women
ATOM demonstrated clinically meaningful BMD gains in men.1,2
For men and postmenopausal women with osteoporosis at high risk for fracture
Not an actual patient.
PROVEN BMD GAINS IN MEN1
TYMLOS was proven to significantly increase BMD in men with osteoporosis in the ATOM trial.1,2
TYMLOS quickly and significantly increased BMD in vertebral and nonvertebral bone.1,2
BMD CHANGE FROM BASELINE TO 12 MONTHS
Placebo (n=79)
TYMLOS (n=149)
(P<0.0001 at all sites)
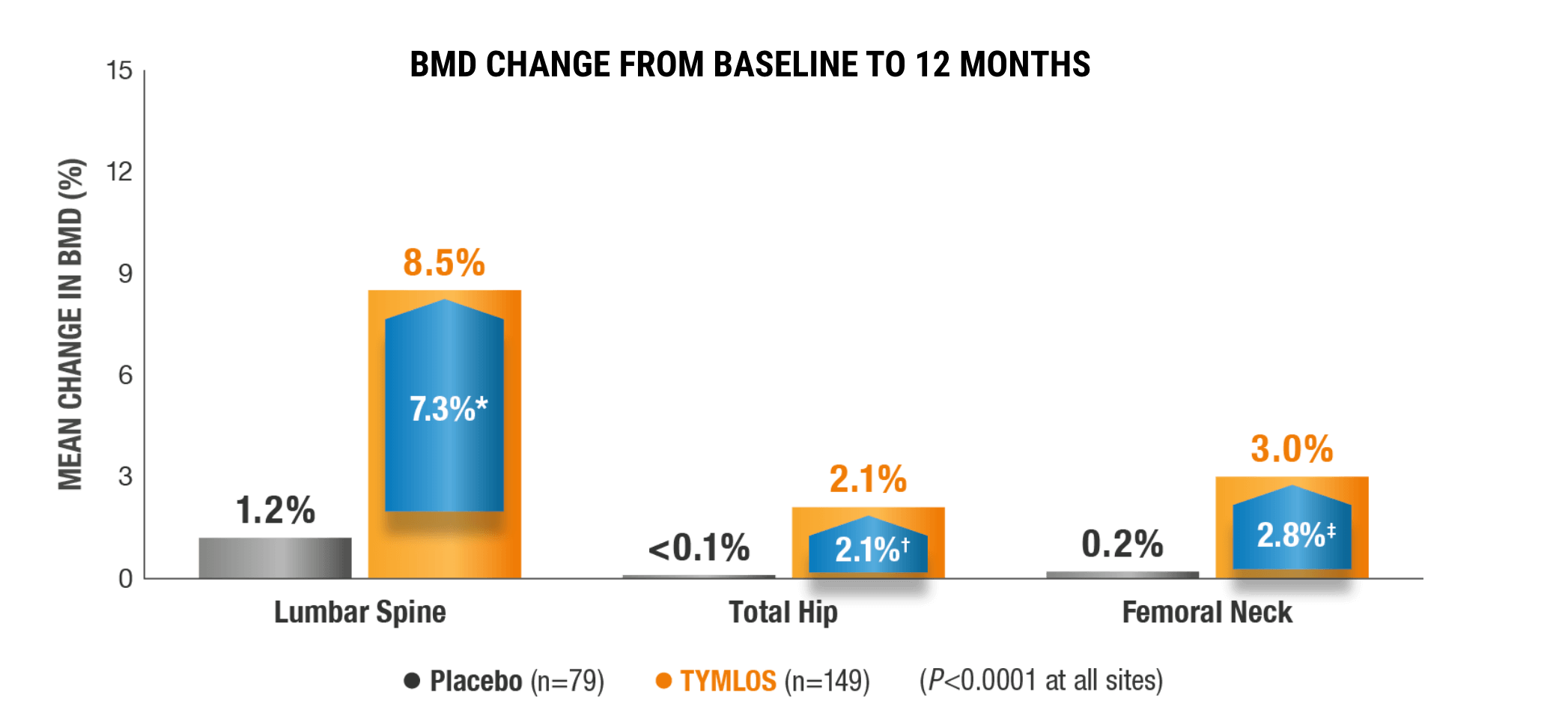
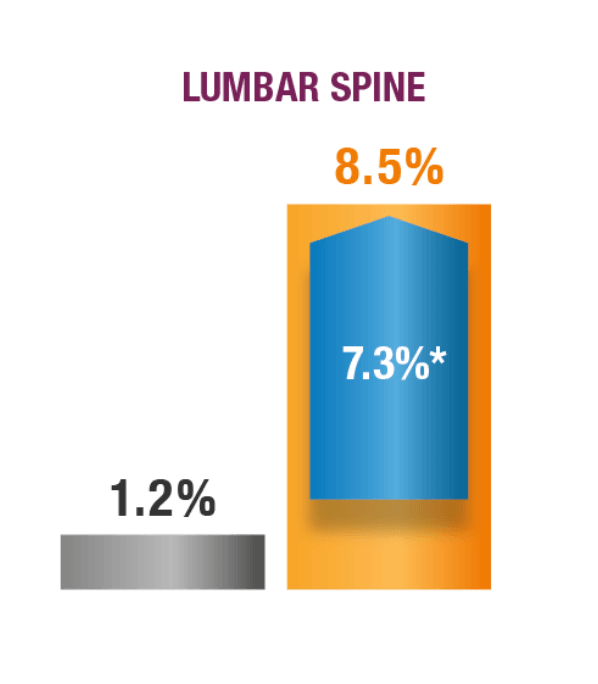
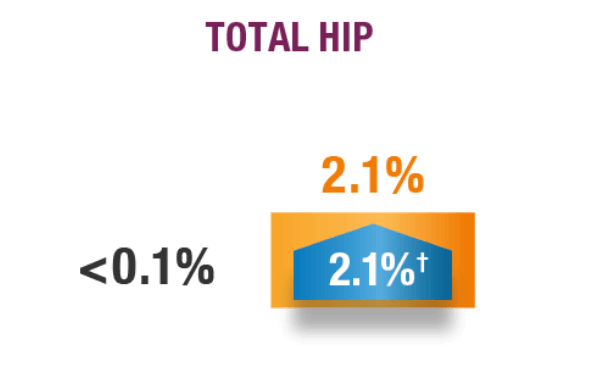

*99% CI: 5.1, 9.6.1
†99% CI: 1.0, 3.2.1
‡99% CI: 1.4, 4.2.1
Higher BMD gains were also observed with TYMLOS at 3 and 6 months.2
| 3 MONTHS (all P<0.01) | Lumbar Spine | Total Hip | Femoral Neck |
|---|---|---|---|
| Placebo (n=79) | 1.1% | 0.2% | 0.2% |
| TYMLOS (n=149) | 3.8% | 1.1% | 1.4% |
| 6 MONTHS (all P<0.0001) | Lumbar Spine | Total Hip | Femoral Neck |
|---|---|---|---|
| Placebo (n=79) | 0.6% | <0.1% | -0.2% |
| TYMLOS (n=149) | 5.5% | 1.4% | 1.5% |
CONSISTENT SAFETY
The safety profile for men in the ATOM trial is consistent with the known safety profile in postmenopausal women with osteoporosis.1
| MOST COMMON ADVERSE REACTIONS* | TYMLOS (n=149) | Placebo (n=79) |
|---|---|---|
| Injection site erythema | 13% | 5% |
| Dizziness | 9% | 1% |
| Arthralgia | 7% | 1% |
| Injection site swelling | 7% | 0% |
| Injection site pain | 6% | 0% |
| Contusion | 3% | 0% |
| Abdominal distention | 3% | 0% |
| Diarrhea | 3% | 0% |
| Nausea | 3% | 0% |
| Abdominal pain | 2% | 0% |
| Bone pain | 2% | 0% |
| Hypercalcemia† | 3% | 0% |
*Adverse reactions reported in ≥2% of TYMLOS-treated patients.1
†Hypercalcemia was defined as albumin-corrected serum calcium of at least 10.8 mg/dL (2.67 mmol/L) at any time point.1
There were no discernible differences in SAEs between treatment groups.
Incidence of SAEs:
TYMLOS: 5.4% vs placebo: 5.1%1
A majority of patients remained on treatment with TYMLOS.
Discontinuation rates:
TYMLOS: 6.7% vs placebo: 5.1%1
Watch Dr. Michael Lewiecki discuss how men are often overlooked when identifying and treating osteoporosis.
See How TYMLOS Offers Flexibility for Patients
IMPORTANT SAFETY INFORMATION
Contraindications: TYMLOS is contraindicated in patients with a history of systemic hypersensitivity to abaloparatide or to any component of the product formulation. Reactions have included anaphylaxis, dyspnea, and urticaria.
Risk of Osteosarcoma: It is unknown whether TYMLOS will cause osteosarcoma in humans. Osteosarcoma has been reported in patients treated with a PTH-analog in the post marketing setting; however, an increased risk of osteosarcoma has not been observed in observational studies in humans. There are limited data assessing the risk of osteosarcoma beyond 2 years of TYMLOS use. Avoid use of TYMLOS for patients at an increased baseline risk for osteosarcoma including patients with open epiphysis (pediatric and young adult patients); metabolic bone diseases other than osteoporosis, including Paget’s disease of the bone; bone metastases or a history of skeletal malignancies; prior external beam or implant radiation therapy involving the skeleton; or hereditary disorders predisposing to osteosarcoma.
Orthostatic Hypotension: Orthostatic hypotension may occur with TYMLOS, typically within 4 hours of injection. Associated symptoms may include dizziness, palpitations, tachycardia, or nausea, and may resolve by having the patient lie down. For the first several doses, TYMLOS should be administered where the patient can sit or lie down if necessary.
Hypercalcemia: TYMLOS may cause hypercalcemia. TYMLOS is not recommended in patients with pre-existing hypercalcemia or in patients who have an underlying hypercalcemic disorder, such as primary hyperparathyroidism, because of the possibility of exacerbating hypercalcemia.
Hypercalciuria and Urolithiasis: TYMLOS may cause hypercalciuria. It is unknown whether TYMLOS may exacerbate urolithiasis in patients with active or a history of urolithiasis. If active urolithiasis or pre-existing hypercalciuria is suspected, measurement of urinary calcium excretion should be considered.
Pregnancy and Lactation: TYMLOS is not indicated for use in females of reproductive potential.
Adverse Reactions:
- The most common adverse reactions (incidence ≥2%) reported with TYMLOS in postmenopausal women with osteoporosis are hypercalciuria (11%), dizziness (10%), nausea (8%), headache (8%), palpitations (5%), fatigue (3%), upper abdominal pain (3%), and vertigo (2%).
- The most common adverse reactions (incidence ≥2%) reported with TYMLOS in men with osteoporosis are injection site erythema (13%), dizziness (9%), arthralgia (7%), injection site swelling (7%), injection site pain (6%), contusion (3%), abdominal distention (3%), diarrhea (3%), nausea (3%), abdominal pain (2%), and bone pain (2%).
- treatment of postmenopausal women with osteoporosis at high risk for fracture (defined as a history of osteoporotic fracture or multiple risk factors for fracture), or patients who have failed or are intolerant to other available osteoporosis therapy. In postmenopausal women with osteoporosis, TYMLOS reduces the risk of vertebral fractures and nonvertebral fractures.
- treatment to increase bone density in men with osteoporosis at high risk for fracture (defined as a history of osteoporotic fracture or multiple risk factors for fracture), or patients who have failed or are intolerant to other available osteoporosis therapy.
IMPORTANT SAFETY INFORMATION
Contraindications: TYMLOS is contraindicated in patients with a history of systemic hypersensitivity to abaloparatide or to any component of the product formulation. Reactions have included anaphylaxis, dyspnea, and urticaria.
Risk of Osteosarcoma: It is unknown whether TYMLOS will cause osteosarcoma in humans. Osteosarcoma has been reported in patients treated with a PTH-analog in the post marketing setting; however, an increased risk of osteosarcoma has not been observed in observational studies in humans. There are limited data assessing the risk of osteosarcoma beyond 2 years of TYMLOS use. Avoid use of TYMLOS for patients at an increased baseline risk for osteosarcoma including patients with open epiphysis (pediatric and young adult patients); metabolic bone diseases other than osteoporosis, including Paget’s disease of the bone; bone metastases or a history of skeletal malignancies; prior external beam or implant radiation therapy involving the skeleton; or hereditary disorders predisposing to osteosarcoma.
Orthostatic Hypotension: Orthostatic hypotension may occur with TYMLOS, typically within 4 hours of injection. Associated symptoms may include dizziness, palpitations, tachycardia, or nausea, and may resolve by having the patient lie down. For the first several doses, TYMLOS should be administered where the patient can sit or lie down if necessary.
Hypercalcemia: TYMLOS may cause hypercalcemia. TYMLOS is not recommended in patients with pre-existing hypercalcemia or in patients who have an underlying hypercalcemic disorder, such as primary hyperparathyroidism, because of the possibility of exacerbating hypercalcemia.
Hypercalciuria and Urolithiasis: TYMLOS may cause hypercalciuria. It is unknown whether TYMLOS may exacerbate urolithiasis in patients with active or a history of urolithiasis. If active urolithiasis or pre-existing hypercalciuria is suspected, measurement of urinary calcium excretion should be considered.
Pregnancy and Lactation: TYMLOS is not indicated for use in females of reproductive potential.
Adverse Reactions:
- The most common adverse reactions (incidence ≥2%) reported with TYMLOS in postmenopausal women with osteoporosis are hypercalciuria (11%), dizziness (10%), nausea (8%), headache (8%), palpitations (5%), fatigue (3%), upper abdominal pain (3%), and vertigo (2%).
- The most common adverse reactions (incidence ≥2%) reported with TYMLOS in men with osteoporosis are injection site erythema (13%), dizziness (9%), arthralgia (7%), injection site swelling (7%), injection site pain (6%), contusion (3%), abdominal distention (3%), diarrhea (3%), nausea (3%), abdominal pain (2%), and bone pain (2%).
- treatment of postmenopausal women with osteoporosis at high risk for fracture (defined as a history of osteoporotic fracture or multiple risk factors for fracture), or patients who have failed or are intolerant to other available osteoporosis therapy. In postmenopausal women with osteoporosis, TYMLOS reduces the risk of vertebral fractures and nonvertebral fractures.
- treatment to increase bone density in men with osteoporosis at high risk for fracture (defined as a history of osteoporotic fracture or multiple risk factors for fracture), or patients who have failed or are intolerant to other available osteoporosis therapy.
References: 1. TYMLOS. Prescribing information. Radius Health, Inc. 2. Czerwinski E, Cardona J, Plebanski R, et al. The efficacy and safety of abaloparatide-SC in men with osteoporosis: A randomized clinical trial. J Bone Miner Res. 2022;37(12):2435-2442. doi: 10.1002/jbmr.4719.
